Congenital Anomalies in Neonates – A Study at Medical College Hospital in Himachal Pradesh
Original Research
Abstract:
The Purpose of study was to find out the overall incidence of clinically detectable congenital anomalies in newborns in hospital deliveries.
All the newborns delivered at Kamla Nehru Hospital, Shimla were examined for congenital malformations over a period of one year. Five thousand nine hundred and ninety seven newborn babies of consecutive deliveries were examined at birth for the presence of congenital malformations. The overall incidence of malformations was 1.63%. Musculoskeletal anomalies were commonly found followed by gastrointestinal and cardiovascular anomalies. The present study was carried out with the aim to determine the overall rate of congenital malformations, incidence in live births, as well as incidence affecting various organ systems, at a medical college hospital in Himachal Pradesh.
Keywords: congenital anomalies, musculoskeletal anomaly, major anomaly.
Introduction:
In a developing country like India due to high incidence of infectious diseases, nutritional disorders and social stress, the developmental defects are often overshadowed, but the present scenario is changing rapidly. Congenital anomalies represent defective morphogenesis during early foetal life. A broader definition includes metabolic or microscopic defects at a cellular level. A recent study shows that congenital anomalies contribute to 9% of perinatal deaths as compared to 8% a decade ago. About 2% newborn infants have major anomalies diagnosed at or soon after birth(1). Congenital anomalies account for 8 to 15%(2, 3) of perinatal deaths and 13 to 16% death in India(4,5).Congenital anomalies can be due to abnormality being either result of genetic constituent or antenatal environment ,plus all condition, known to be caused by specific genes at whatever age they become manifest and whether or not they are associated with a demonstrable abnormality of form(6,7).
Major anomaly is defined as an anatomic abnormality severe enough to reduce normal life expectancy or compromise normal function e.g. heart defect, spinal defect, intestinal defect(8).Major anomalies have serious medical, surgical and cosmetic consequences.
Minor anomaly is a physical feature often familial that is present in only a small proportion (1 to 5%) of normal individuals e.g. simian crease of palm ,epicanthal folds(8).
Incidence and geographical distribution of congenital anomalies:
The worldwide incidence of congenital disorders is estimated at 3-7% but actual number varies between countries. Population and hospital based studies from different parts of India show that 2.5% of newborns have birth defects. Even here pattern of malformation varies from region to region e.g. Neural tube defects are common un northern India as compared to musculoskeletal defects are more common in rest of India(9).
Aims and Objectives:
1) To study the overall incidence of clinically detectable congenital anomalies in newborns in hospital deliveries.
2) To classify the congenital anomalies in major and minor groups.
Material and Methods:
It’s a prospective observational type of study. Study population consisted of five thousand nine hundred ninety seven babies delivered at the Department of Obstetrics and Gynaecology,Kamla Nehru hospital, Shimla who were examined at birth for the presence of congenital malformations. All the newborns were looked for major and/or minor congenital malformations and everyday during routine ward rounds. Relevant information regarding maternal age, gestational age, sex, community, birth weight, birth order and consanguinity was documented. Significant antenatal history like maternal illness, ingestion of drugs, exposure to radiation and complications during labour was recorded. Antenatal ultrasonography (USG) findings were noted. Relevant radiological, histo-hematological tests were carried out. Baby’s gestational age, birth weight, sex and symptoms in postnatal period were noted. The detailed general and systemic examinations of the babies were carried out. Thorough physical examinations of newborn babies were done. All macroscopically anatomical defects were recorded in a predesigned Performa. A meticulous general and systemic examination was carried out by a consultant at the time of birth to detect any malformations. Ultrasound was employed routinely to detect multiple congenital anomalies and to rule out majority of the internal congenital anomalies. 2D echocardiography was also used for all congenital heart diseases, along with the routine X-ray chest and electrocard-iogram. Those babies who were born with any external malformations were subjected to relevant investigations to rule out internal anomalies. Malformations were categorized in major and minor defects. The major malformations were divided into central nervous system (CNS), musculoskeletal, gastrointestinal, genitourinary, cardiovascular system (CVS), syndromes and miscellaneous disorders.
Observations:
During period of one year, total 5997 deliveries were conducted, 5867 were live births and 130 were stillbirths. The number of babies with congenital malformations diagnosed at birth or within the first week of life was 77, while the total number of malformations was 96 (1.63%).
Table I and II give the sex distribution and incidence of congenital malformations. The sex wise distribution was 39 males and 38 females, giving an M: F ratio of 1.02:1, while p value was 0.6062 which was not statistically significant.


Incidence of malformations in general was found to be apparently more in female (1.38%) than in male (1.24%).
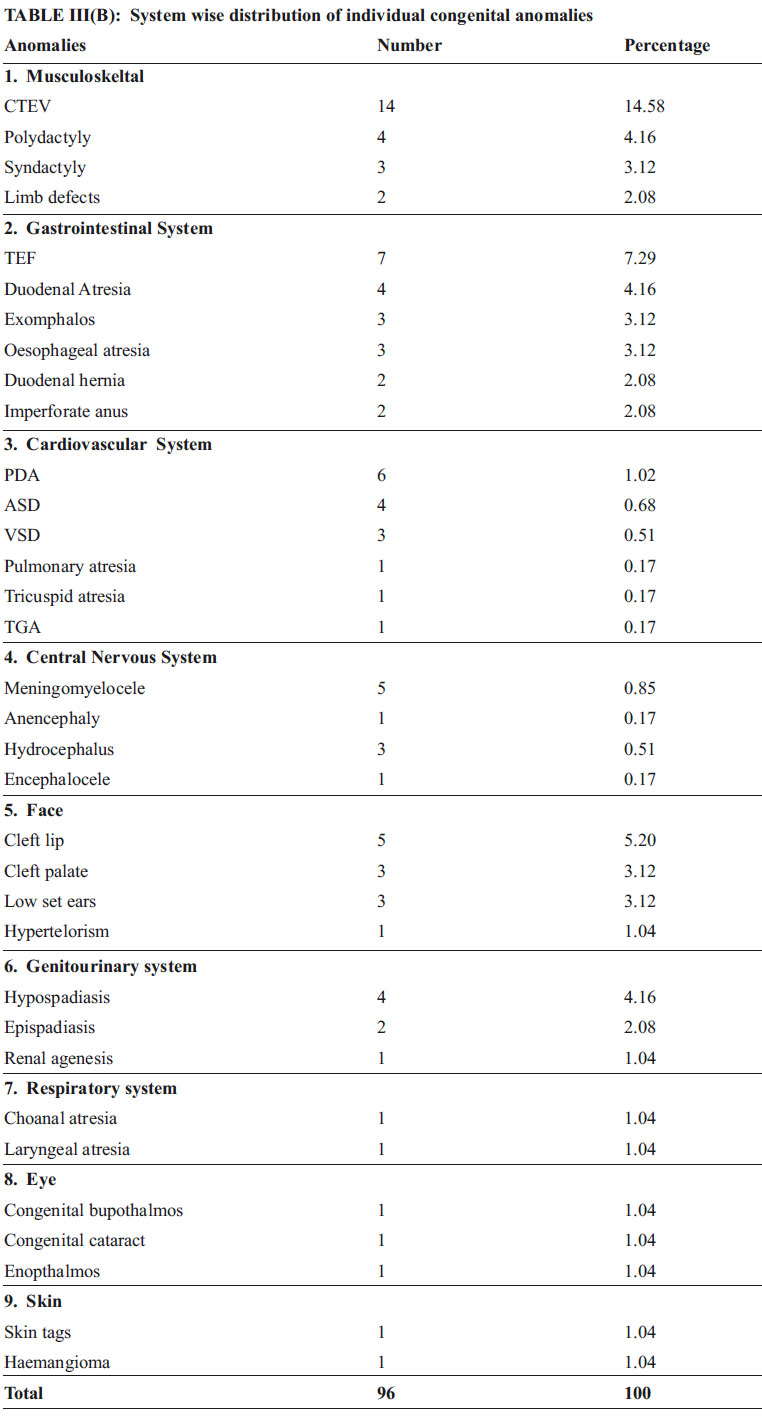
Pattern Of Congenital Anomalies :Musculoskeletal system was the most common system involved accounting for 23.84% of total congenital anomalies followed by decreasing frequency as cited in Table III. Of the 96 anomalies, there were 83 major anomalies and 13 minor. In the major anomalies Musculoskeletal anomalies were commonly found followed by gastrointestinal and cardiovascular anomalies. In the minor anomalies polydactyly was the most common followed by syndactyly and low set ears.

Higher frequency of congenital anomalies was seen in the babies born with low birth weight however P value not being significant as shown in Table IV.

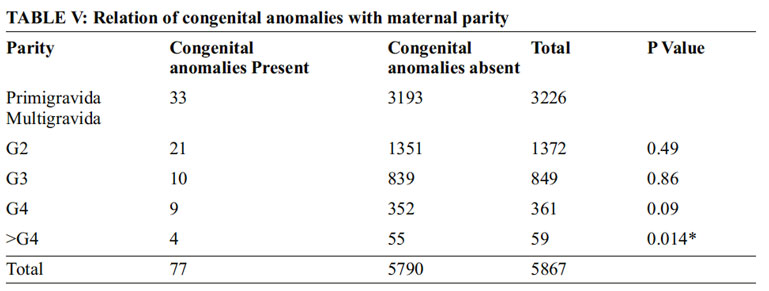
There were higher number of congenital anomalies in babies born to mothers in the age group 20-30 yrs of age (74%) and next in order were > 30 years accounting for (18.2%),least number of congenital anomalies were in the babies born to age less than 20 years. P value was not significant. Incidence of congenital anomalies was higher in multigravida as compared to primigravida. The incidence increased as the parity increased as shown in Table V. P value was significant (<0.0.5) and in multigravida (>Gravida 4)
Discussion:
Congenital anomalies are important causes of still births and infant mortality, and are contributors to childhood morbidity. The number of birth defects in infants is increasing antenatally and during the neonatal period due to advanced diagnostic technology, especially USG. The incidence in the present study is lower than as reported by studies quoted in table below, this difference may be due to the fact because in the present study only live newborns have been taken and still born have been excluded. Other factors can be different culture, geographical conditions, inaccurate detection at birth, period of observation, autopsy rate as in certain centers autopsies have been performed and this leads to higher incidence in some studies. Other factors which can contribute to the difference in the incidence like genetic factors, geographical area of settlement, socioeconomic status ,maternal nutrition and habits, prenatal health care services and large number of environmental factors which could not be measured.

Association of low birth weight with increased risk of congenital malformations was very well documented15, our study was in accordance with this. The incidence of congenital anomalies was significantly higher in term babies as compared to Pre term babies. Male preponderance amongst congenital malformed babies was found in this study which was statistically insignificant.
In present study no consanguinity was recorded. Previous studies have15reported that significantly higher incidence of malformation among the mothers of gravida 4 or more and our results are consistent with this finding. This indicates that as the birth order increases, the incidence of congenital anomalies also increases. Certain maternal diseases may occasionally lead to increased risk of birth defects. According to Ordonez et al., 16 diabetes mellitus, arterial hypertension, and hypothyroidism show a positive association with congenital malformation. In our study Antenatal history of mothers were suggestive that 45.5% were anemic, 13% had hypertension and 3% had gestational diabetes mellitus.
With regard to pattern of congenital malformations in present study the system involved in descending frequency were musculoskeletal (23%), followed by gastrointestinal system (21%) and cardiovascular (16%),face(12.45%),CNS (10%) and genitourinary system (7.2%).In the present study congenital anomalies involving musculoskeletal system were found in 23.7% with an incidence of 3.92 per 1000 live births, talipes was the most common anomaly.
As musculoskeletal anomalies anomalies were most common in our study reason being that these anomalies are externally visible hence were easily picked up. Internal organs (gastrointestinal system, cardiovascular system) anomalies were less detected because of invisible nature of the systems and also neonates have been asymptomatic in particular during first 24 hours of life. Other reasons are lack of follow up.
With regard to the cardiovascular system, patent ductus arteriosus was the most common lesion followed by atrial septal defect and last being ventricular septal defect. Among the genitourinary tract anomalies, hypospadias, was the most prevalent lesion. Regarding the central nervous system, the most prevalent anomaly encountered was meningomyelocele seen in 5.2% cases and congenital hydrocephalus found in 3.12% cases. With special reference to the neural tube defect (NTD), the incidence of NTD has markedly reduced in the developed countries following mass promotion and mandatory prescription of folic acid for pregnant mothers.17-20
Incidence of facial anomalies was 2.04 per 1000 live births, percentage being 12.4% among other congenital anomalies. Cleft lip most common followed by cleft palate and low set ears. Incidence of cleft lip and palate in present study was 1.21 per 1000 live births. V. Dutta12(2000) recorded cleft palate as the most common anomaly but it has been cited in gastrointestinal tract anomalies.
Conclusion:
Congenital anomalies are a major cause of stillbirths and infant mortality. By thorough clinical examination, the life-threatening congenital malformation must be identified, as early diagnosis and surgical correction of the malformed babies offer the best chance for survival.
Conflict of Interest – None
Source of Funding – Nil
Contribution of authors-Vijay Yadav:
Conducted the study under supervision,
Rakesh Sharma: Chief supervisor and guide,
Jyotsna Sharma: Assisted the study,
Pancham Kumar: Co guide,
Deepak Sharma: Biostatistics and manuscript.
References:
1. World Health organization, world health report 1998. Ganeva WHO 1998;43-47.
2. Ravikumara, M. & Bhat, B.V. Indian J Pediatr (1996) 63: 785.
3. Kumar, M.R., Bhat, B.V.&Oumachigui, A.Indian J Pediatr (1996) 63: 357.
4. Chaturvedi P1, Banerjee KS. An epidemiological study of congenital malformations in newborn. Indian J pediatrics 1993; 60;645- 655
5. Aggarwal SS , Singh V,Singh PS, Singh SS et al.Prevalence & spectrum of congenital malformations in a prospective study at a teaching hospital. Indian J Med Res 1991; 94; 413-419.
6. M.M. Nelson, J. O. Forfar. C ongenital Abnormalities at Birth: their Association in the same Patient. Developmental medicine child neurology1969; 11:3-16.
7. Potter EL. The effect on foetus of viral disease in mother .Clin Obstet Gynaecol1961; 4;327- 340.
8. Maclean DS .Congenital malformation. In: MacDonald MG, Mullet MD et al.Avery’s Neonatology: Pathophysiology & Management of the Newborn,5th ed. Philadelphia Lippincott;1999.p.839-859.
9. Park k. congenital malformation. In K Park(ed).In Park’s tectbook of preventive and social medicine.15th edition;2005:379-80.
10. Chaturvedi P, Banerjee KS.Spectrum of congenital anomalies in the newborn from rural maharashtra. Indian J pediatrics 1989;56:501-507.
11. Swain S,Agarwal A,Bhatia BD.Congenital Malformations at birth.Indian Pediatr 1994;31:1187-1191.
12 Dutta V,Chaturvedi P. Congenital malformations in rural maharashtra.Indian Pediatr 2000;37:998-10001.
13. Desai AN, Desaai A. Congenital anomalies -A prospective study.bhj 2006;4803:442-445.
14. Singh A,Gupta RK.Pattern of congenital anomalies in newborn:A hospital based prospective study.JK science 2009;11:34-39.
15. Mohanty C, Mishra OP, Das BK, Bhatia BD, Singh G. Congenital malformation in newborn: A study of 10,874 consecutive births. J Anat Soc India. 1989; 38:101-11.
16. 9. Ordóñez MP, Nazer J, Aguila A, Cifuentes L. [Congenital malformations and chronic diseases of the mother. Latin American Collaborative Study of Congenital Malformations (ECLAMC) 1971-1999] Rev Med Chil. 2003;131:404-11. [PubMed]
17. O’Dowa MJ, Conolly K, Ryan A. Neural tube defect in rural Ireland. Arch Dis Child. 1987;62:297-8.[PMC free article] [PubMed]
18. Singh R, Al-Sudani O. Major congenital anomalies at birth in Benghazi, Libyan Arab Jamahiriya, 1995. East Mediterr Health J. 2000;6:65-75. [PubMed]
19. De Wals P, Trochet C, Pinsonneault L. Prevalence of neural tube defect in the province of Quebec, 1992. Can J Public Health. 1999;90:237-9. [PubMed]
20. Martinez-Frias ML, Bermejo E, Frias JL. Analysis of deformations in 26,810 consecutive infants with congenital defects. Am J Med Genet. 1999;84:365-8. [PubMed]
Issue: January-March 2017 [Volume 6.1]
