DIAGNOSIS AND MANAGEMENT OF CHRONIC CONSTIPATION
Review Article
Abstract:
Constipation is a common problem in childhood, often presenting in chronic form. Unless it is organic, mostly encountered in early infancy, most of the times its exact cause is not established despite all possible investigations. As many of these are non-contributory, are in fact not necessary. When no cause is found, the diagnosis is conventionally described as ‘Functional Constipation’ although there is no actual psychological element attached to it. Besides discomforts, recurrent pain abdomen, growth failure and understandable social embarrassment, the treatment is a long drawn process, demanding understanding of all stakeholders – the child, parents and Paediatrician. Not only it is desirable to add more fiber to diet, plenty of fluids, active life style, most children would need maintenance laxative for pretty long. This has to be well explained to the parents and caregivers for successful outcome.
Key words:
Functional constipation, encopresis, slow transit constipation, ROME III criteria, anal fissure, hard stool, Hirschprung’s disease, fiber diet, PEG, lactulose, Bio-feedback, rectal manometry, Behaviour modification
Introduction:
Constipation is a very common problem encountered in day-to-day paediatric practice. It is one of 10 most common conditions encountered, seen among 3% in general pediatric OPD and about 20 to 25% in specialty (PGE) clinics1,2. Of these, 1.3 to 5% cases are accompanied by encopresis, a great embarrassment and anxiety to both child and parents2. The current trend of sending the tiny tots under 3 years to kinder- garden school early in the morning, even their bladder and bowel control is fully established, not to talk of the toilet training, has compounded the problem tremendously.
Definition:
Constipation is subjectively described as delay or difficulty in defecation for last two weeks or more, sufficient to cause significant distress to child. In Objective term, it is the passage of stool less than 3 per week with or without encopresis more than once per week1 or large volume stool once in a week to a month so as to clog the toilet with palpable mass felt P/A or P/R. Constipation is conventionally Classified3 as (A) congenital and (B) acquired, depending upon the age of onset; and as acute (2-8 weeks) and chronic (>8 weeks), depending upon its duration.
PaCCT4 Diagnosis Criteria for chronic constipation: Must satisfy any two of the following:
1. Frequency of bowel movement less than 3 per week.
2. > 1 fecal incontinence per week.
3. Palpable fecal mass per abdomen or through P/Rectal examination.
4. Passed large volume of stool so as to clog the toilet.
5. Retentive posturing / with– holding behavior
6. Painful defecation
In more than 90 to 95% of cases of acquired variety, the cause is not established. Hence it is described as ‘functional’ constipation, often used synonymous with chronic constipation, manifesting either in mild or severe forms.
Rome III5,6 Diagnosis criteria of functional constipation: Must satisfy any 2 of following:
1. Two or fewer (<3) defecations per week.
2. At least 1 episode of fecal incontinence / week after child acquires toilet skills.
3. History of excessive stool retention or retentive posturing.
4. History of painful or hard bowel movements.
5. Presence of a large fecal mass in the rectum.
6. History of large diameter stool that may obstruct the toilet.
In infant and children up to a developmental age of 4 years, these symptoms may be present for at least one month. In over 4 years old, child should be symptomatic for at least two months, with insufficient criteria for diagnosis of Irritable Bowel Syndrome6.
However, it could be just the tip of the iceberg. Hypoganglionosis7 is said to comprise 3- 5% of gastrointestinal innervations defects, resulting in resistant chronic constipation. In oligoneuronal dysganglionic hypoganglionosis, myentric ganglia are of normal size initially, having normal interganglionic spacing and normal neuronal contents. These nerve cells happen to be hypoplastic and the ganglia undergo progressive nerve cell loss, eventually progressing to atrophic hypoganglionosis, morphologically similar to hypoplastic hypoganglionosis. This results in decreased acetylcholine esterase activity in the nerve fiber network at muscularis propria.
Further, slow transit constipation (STC) is a form of chronic constipation with delayed colonic stool passage. Etiologies include reduced neurotransmitter levels, reduced interstitial cells of Cajal (ICC) density, or connective tissue (CT) synthesis. Chunk of such cases might be contributing significantly to the functional group, as advanced investigations like manomerty, mucosal biopsy are neither routinely done nor warranted.
5-10% of acquired variety are secondary to:
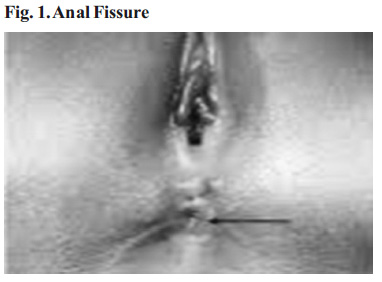
1. Anal lesion – Fissure (Common in infants and toddlers on formula or following diarrhea, Fig. 1), meconium plug, anal bands, abscess, strictures (CBD, TB), surgery and local injury. Resulting pain and withholding thus leads to constipation and impaction of hard stool. This leads to megarectum or mega colon, formation with faecolith, recurrent pain abdomen and at times, solitary ulcers in rectum1.
2. Neurologiacal conditions: Cerebral palsy, mental retardation, hypotonia, meningomyelocele, tumors or tethered spinal cord, cauda equine sundorme.
3. Metabolic / genetic – Hypokalemia, hypomagnessemia, hypophosphatemia, hypercalcemia, cystic fibrosis, celiac disease, obesity.
4. Endocrine:Hypothyroidism, diabetes, hyperparathyroidism
5. Drug induced: Antimony, Aluminum, Calcium, Iron, Lead, Bismuth, Barium, Mercury, Antimony, Anticholenergics, sympathominetics, antacid, anti HTN, NSAID, anti epileptic, codeine, opiates, phenothiazines, methyl phenidate, antidepressants and calcium channel blockers etc.
6. Dietary: Low fiber, junk food, beverages, ketogenic diet, dieting, anorexia.
7. Psychogenic, IBS, laxative abuse, limited toilet access.
Fecal soiling:
It is defined as, “Involuntary and voluntary passage of stool in the under-wear under 4 years of age in a socially inappropriate place or circumstance.” Under this broad heading, Encopresis1 needs to be differentiated from fecal incontinence, which is basically due to some anatomic defect. Encopresis could be functional or as a consequence of chronic constipation (Overflow) where fecal mass could occupy rectum, sigmoid colon, ascending or even the whole of colon and there is decreased ability to sense stool volume (Chronic rectal or colonic distention increases perception of pressure threshold secondary to with- holding).
Incidence:
Normally breast feed infants pass more frequent (5 to 6) stools than formula-fed, may be with each feed, due to gastro-colic reflex. The transit time during 1 to 4 months of age is approximately 8.5 hours, reaching 30 to 48 hours by adult-hood. By 4 months, all infants passed an average number of 2 stools (range 1 to 7), irrespective of the type off feed which reduces to 1.2 stools in an average after 4 years of age1, 8. In a study covering 560 constipated patients9. Their age distribution was: Infants (19.1%), preschool (42.9%), school age (26.9%), and adolescents (11.0%). There was no gender difference among these 4 groups. Less than 3 bowel movements per week was observed mere frequently in pre-school (65.8%) and school age (59.6%) than infant (52.4%) and adolescents (43.1%). Fecal soiling was in 75.6% of the pre-school aged > 48 months, in 68.2% of school age and in 76.7 % of adolescents. Soiling was more frequent among boys (80.7%) than girls (50.0%). Retentive posturing (67.6%, 40.7%, 27.2%), fear for defecation (70.2%, 44.2%, 29.7%), and abdominal pain (80.8%, 69.6%, 73.6%) were encountered frequently in pre-school than school age and adolescents.
Approach:
History taking
It is most important; including birth history, feeding, weaning, introduction of cereals, development milestones and other aspects to establish / rule out any congenital or secondary condition. An infrequent stool pattern is present in the beginning with decreased frequency, withholding, abdominal distention, pain and relief after defecation. Cycle of blunted appetite, poor or no weight gain, passage of hard balls/ pellets, large volume stools, clogging toilets, typical posturing, recurrent UTI may ensue. Stool charting is useful. Questioning of parents is important – frequent of defecation, consistency, and associated behavior etc in order to confirm that child’s real problem is constipation.
Physical examination:
From anthropometry to systemic examination; including inspection of lumbar, sacral regions for dimpling, scars, tufts of hair, asymmentry, anoucutaneous reflex, P/R examination for anal tone, stenosis, anal fissure (Fig.1), rectum contents at rest and then while child tries to squeeze, push in order to detect paradoxical contraction.
In a Sri Lankan study10 using Rome III criteria, out of 2694 school children studied, 416 (15.4%) were diagnosed as ‘Functional Constipation’. Independent symptoms associated were straining (71.6% Vs 28.4% of controls), bleeding per rectum (14.2% Vs 2.2%) and abdominal pain (55% Vs 35.2%). Significantly higher was positive family history of constipation (49% Vs 14.8%), living in a war zone (18.1% Vs 13.7%) and attending urban schools (16.7% Vs 13.3%).
In a community-based study11 in Brazil, prevalence of functional constipation among 536 children under 11 was 17.5%. Straining as the complaint of highest sensitivity fir diagnosis (96.8%) while pain to defecate was of highest specificity (99.5%). Among 78 children (Mean age 4.6 years, 62% boys) having chronic constipation, functional constipation was the most frequent cause (62.8%), followed by Hirschsprung’s disease (24.3%). The study inferred that while functional constipation remained the most frequent cause of chronic constipation, Hirschsprung’s disease is the number one organic cause, warranting the need of rectal manometry for diagnostic confirmation.
In a hospital based retrospective study12 from medical records at SGPGI, Lucknow, out of 137 cases of constipation (M:F::90:47), 117 (85%) were functional constipation and 20 (15%) were of organic cause. Hirschsprung’s diseases were 6%. Most had delayed passage of meconium (50.0% Vs 1.7%) at birth, symptoms since 1st month of life (40.0% Vs. 1.7 %), abdominal distension 50% Vs. 5% in functional group. Among the functional group, fecal impaction was in 20%, straining in 35%, withholding in 27.4% and incontinence in 30.8%. 95% responded to laxatives where as10% needed disimpaction.
In a recent study from middlle-east13 on children aged below 18 years of age using ROME III criteria after excluding functional constipation, abdominal pain, fecal mass, rectal bleed, anorexia, fecal soiling, retentive posturing, withholding, anal fissure, peri-anal erythema were recorded. Of 222 children (M:F 98:124 and mean age was 5 ± 3.12 Years), mean duration of constipation was 2.2±1.9 years. Large, hard stool in 93.7%. Painful defecation and with-holding in 92.3% and 91.9%, respectively. Fecal impaction were frequent among boys than girls (p<0.01). Fecal soiling was in 40.8% of boys, 28.2% of girls (p=0.04). Fresh rectal bleeding, anal fissure were least frequent.
In our own experience in a prospective hospital based study14 (Ongoing, unpublished), of 118 cases of constipation, 100 (83.3%) were diagnosed as functional constipation based on ROME III criteria after excluding organic aetiology. Many of them were in 4-6 year age group (Range 1-10 Years), none below 1 year. We encountered reduced appetite in 8%, weight loss 6%, stool frequency 2 or less per week 31%, Pain abdomen 13%, Pain while passing stool 21% hard stools 8%, Bleed while defecation 3% and faecal soiling 8%. On examination, 31% were anemic, 18% had liver enlargement and 2% anal fissure. There was no congenital anomaly or any neurological deficit. There were only 3% cases who were having TSH marginally higher but ormalised on follow-up. Most cases exihibitted chronic undernutrition. Their height varied between 80% to 90% of expected for age, weght for height from -1 to – 2 SD and BMI between -2 to -3 SD (Table 1, 2).

Quality of life:
In a study15 comprising of 100 children having chronic constipation, all were evaluated for their quality of life by questionnaire method by a 0- 100 scale contained in parents CHQ- PF50 in terms of physical and psychological parameters. Both these aspects of health were found to be significantly lower, compromising quality of life as compared to normal.
Investigations:
Plain AxR (KUB), Ba enema (Fig. 2, 3, 4) and USG are valuable tools. In selected cases, rectal biopsy, thyroid function, Calcium / PO4, colonic transit time, manometry, motility studies, peri-anal electro-myography, defecography, sweat chloride, anti-gliadin antibody etc may be required.

USG: A new USG scoring system, designed to assess the fecal loading and its effect on the bladder has been used16. 500 patients (male317, female 183; median age 8 years; in age range 8 month to 18 month) completed a’ standardized symptoms severity score sheet’ (SSS) for constipation. The USG done placing probe 2 cm above the public symphysis, followed up for four subsequent visits. Correlation between SSS and US findings measured. It was inferred that US was an easy and quick tool in out -patient setting to assess severity of constipation. The scoring system was found to be a reliable in conjunction with clinical examination for assessing long-term outcome.
In another prospective double blind study17 comprising of 132 children with constipation, gallbladder motility disorder was identified in the group with severe constipation as compared to their age and sex matched controls of same number.
Hydro-colonic echography18:
263 children with chronic constipation, aged between 14 days and 17 years were evaluated. Position of colon, lengthening and lumen, structure of intestinal wall, haustra, real time functioning were studied. Secondary changes in colon were noted, depending on intensity of constipation. Echo characteristics of mild or severe constipation, echoidentification of surgical conditions like- Hirschsprungs, identifying organic etiology are the advantages. This narrows down additional investigation in the functional group, identifies secondary changes in colon due to long standing constipation. It serves as a quality control of conservative treatment also. There is no radiation and its unlimited replication is the added advantage.
MRI: In a study19 to determine the prevalence of lumbosacral spine ( L S S ) abnormalities in children with defecation disorders, intractable constipation or non-retentive fecal incontinence, MRI showed LSS abnormalities in 3% of patients with defecation disorders and normal neurosurgical intervention. Thus, whether or not LSS abnormalities play a role in defecation disorder remain unclear.
The Latin-American consensus on chronic constipation recommended use of barium enema as an initial investigation only in countries with a high prevalence of idiopathic mega colon or Chagas disease20. Complimentary investigations such as colonic transits followed by ano-rectal manometer and defecography were only recommended to rule out colonic inertia and / or obstructive defecation in patients not responding treatment. Biofeedback was recommended (grade B) for those with pelvic dys-synergia.
Management:
Multi- modality approach.
1. Counseling, education and retraining
2. Treat the underlying cause, if any after due investigations.
3. Disimpaction or evacuation
4. Maintenance therapy
5. Follow-up
Counseling, education and retraining of parents, care givers and child:
It is required to re-emphasise that constipation is a symptoms complex, not a disease. The anatomy and patho-physiology must be explained in simpler words. (Fig. 5)
All available treatment modalities, duration etc need to be discussed for their informed choice, co-operation and active participation. Both need to understand the involuntary process that leads to fecal incontinence. The accompanying anxiety on their part is understandable, so also the attitudes of guilt or blame which must be addressed.
Conditions like anal fissure (Fig. 1) need alleviation of pain by at least twice a day application of a local anesthetic agent. For simple constipation, only general measures like good hydration, high carbohydrates, fiber rich diet are necessary. Leafy and green vegetables, toilets retraining and at the most, a laxative / stool softener like milk of magnesia or lactulose for a week or ten days would suffice after initial counseling. No enema is required for evacuation.
Chronic constipation demands aggressive therapy in a planned manner by a multi – disciplinary team, in addition to above measures. The Latin American consensus21 recommended an increase in dietary fiber up to 25.30 g per day (grade C). No evidence was found to recommend measures such as exercise, increased water intake and frequent visits to the toilet. Fiber supplements such as Psyllium had received grade B recommendation and pharmacotherapy with tegaserod, polyethylene glycol, both got grade A. There was insufficient evidence to recommend lactulose, but the consensus did not object to its use when necessary. It was found that 75% used some type of medication, with more than 50% resorted to home remedies.
Disimpaction and maintenance:
When chronic constipation is severe or is associated with impaction, mega colon, mega rectum or encopresis, aggressive management is warranted.
Disimpaction is preferred using oral polyethylene glycol non-electrolyte solution22 in the dose of 1.5 gm per kg of body weight, dissolved in 200 ml of water once daily for 3-4 days, followed by a maintenance once daily dose of 0.26 – 0.8 gm per kg, dissolved in 100 water for about 6 months to allow the dilated, over-stretched rectum / colon to structurally and functionally return to its normal shape and perceiving usual pressure threshold.
Alternatively, per-rectal enema of hypertonic sodium phosphate23 (Neotonic enema) in the dose of 6ml per kg per day 12 hourly for 2 days, followed by maintenance therapy with oral PEG is the practice at many centers including ours, with satisfactory outcome. A stool softener like lactulose has also been used for maintenance but risks tolerance after few days, produce bloating and demands adequate hydration.
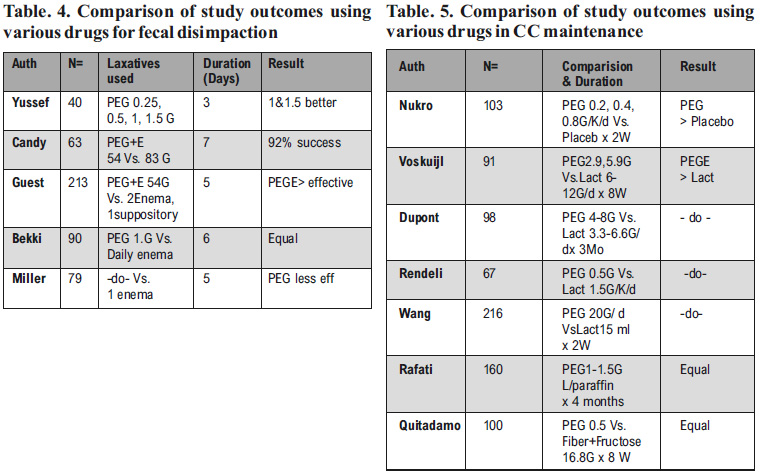
A randomized controlled trial when compared polyethylene glycol (PEG 3350) with lactulose in 100 children aged 6 month to 15 years, over eight weeks24 the treatment was significantly more effective in PEG group than in lactulose group (56% Vs. 29 %) with very few adverse effect. A second study confirm the clinical and biological tolerance of PEG in children treated for 3 month and found it better than lactulose side effect25, 26 such as flatulence and vomiting. In our own ongoing study it was established that daily dose of 0.3G/K was sub-optimal14 as compared to 0.8G/Kg/day dose (Table 3). Results of crossing over the dose between the groups is underway. A comparision between various studies using PEG, lactulose, milk of magnesia for dis impaction and maintenance separately are given in Tables 4 and 5 respectively27.
Conventional treatment regime effective in colonic dysmotility.
This Brazilian study28 included 34 children with functional constipation. Total and segmental colonic transit times were assessed using radioopaque markers. Hydrogen breath test was used to evaluate lactulose and mean oro-cecal transit time. Treatment consisted of disimpaction, general measures, dietary fiber intake and mineral oil administration. Colonic dysmotility was found in 71.9% (23/32). All showed improvement after 6 weeks of treatment. 82.6% (19/23) with dysmotility returning to normal or reduced the severity in eight week of treatment. Lactulose orocecal transit time decreased (70 to 50 minutes, p=0.002), bean oro-cecal transit (240 to 220 minutes, p=0.002), and total colonic transit (69.5 to 37.0 hours, p= 0.001). It proved that conventional therapeutic approach yielded good results regardless of presence or absence of colonic dysmotility. Hence, gut motility abnormalities in functional constipation in children do reverse, which could be secondary to constipation itself.
Toilet retraining
Usually there exists a faulty or improper toilet training before hand among these kids. Squatting in an Indian type of toilet is best option for allowing the concerned muscles to act effectively while facilitating gravitational force to supplement the defecation process. If sitting on an European commode, the child’s feet must rest on appropriate support so that combined with the action of levator ani, and positioning, the axis of rectum and anal canal are aligned together to facilitate defecation. (Fig. 5) The training program should simultaneously start with treatment of constipation, whatever kind it may be. The child may be fearful of painful defecation and parents must understand that the toilet training in the given situation may not be successful but paying subsequently. The child should be persuaded by parents to sit in the toilets 10 to 15 minutes after having breakfast at least for 10 minutes daily as a matter of habit, irrespective of the outcome. Having woken up late, having a little or no catch the school bus has been too much these days for a tiny – tot. It has come in a big way disrupting the system badly.
Behavior modification:
It is an important element of management that can be effectively delivered on OPD basis. Regular and unhurried toilet habits encouraged. A reward point system evolved for successful use of the toilet, clean pants etc. a dairy stool frequency is insisted upon.
Bio- feedback is feasible when child is at least 5 years old to understand and co- operate. In older children, faecal incontinence and its social embarrassing situations needs a clear no blame sympathetic approach.
Follow–up:
It is required to monitor progress with treatment (Minimum 6 months to about 2-3 years) and for prevention of relapse24. Re-enforcing diet rich in carbohydrates and fibers, plenty of fluids, exercise, toilet training, avoidance of beverages, junk food are essential. Intensive follow-up required in problem cases like CP, intellectual disability, neurological disorders, hearing impaired, disobedient, teen onset, substance and alcohol abuse where prognosis is challenging. Early referral to specialized centres desirable for advanced investigation and appropriate management when an organic aetiology is suspected.
Surgery: Continued failure to respond to treatment may require surgical intervention, although rarely. Caecostomy and antegrade continence enemas reduce frequency of soiling and abdominal pain in children with slow transit constipation.
Summary:
Chronic or functional constipation is a common problem in childhood, with soiling a significant issue. Explicit criteria for the diagnosis of constipation and a defined terminology now exist. The morbidity is high and the treatment is complex. There is a very poor evidence base for the base for the drug treatments used and there are considerable differences in practice. Key to successful management is early diagnosis, prompt and sustained treatment with emphasis on holistic care, having multidisciplinary support. Non-drug aspects of care, including patient education and behavioral modification, besides use of an appropriate laxative, are the first line therapy. Management is based largely on clinical experience and consensus.
References:
1. Rita Stephen and Vera loaning Baucke. Constipation and Encoprssis in willie/ Hyams eds Paediatrics GI Dis 2nd edn; 1999, W.B Saunders Co.
2. Beniga MA et al. Childhood constipation: is there new light in the tunnel? JPGN2004,39:448-464
3. Thapa B.R. Constipation and encopresis in infant and children: Selected topics in pediatrics for practioners Ed. A. Parthasarathi. Pub. Jaypee, 1st Edn 2004, 147- 159
4. Benninga M,et al. The Paris consensus on childhood constipation terminology ( PACCT) Group. JPGN 2005;40:273-5.
5. Hyman PE, Milla PJ, Benninga MA, Davidson GP, Fleisher DF, Taminiau J. Childhood functional GI disorders: nenonate / toddler. Gastroenterology 2006;130:1519- 26.
6. Rasquin A, Di Lorenzo C, Forbes D, Guiraldes E, Hyams JS, Statano A et al. Childhood functional GI disorders: Child / adolescent Gastroenterology 2006;130: 1527-37.
7. Bruder E, et al. Hypoganglionosis as a cause of chronic constipation. Der Pathology 2007, 28 (2) : 131-6
8. Motta ME, silva GA. Chronic functional constipation in children: diagnosis and prevalence in a low- income community. 2. Jornal de pediatria ; 1998, 74(6) : 451-4.
9. Boukthir S, et al. chronic constipation in childhood. A report of 78 patients . La Tunisie Medicale ; 2007,85(2) : 109-15
10. Rajindrajith S et.al constipation in children an epidemiological study in Sri Lanka using Rome III criteria. Archives of dis in childhood 2010.
11. Fontana M, Bianchi C, Cataldo F, Conti Nibali S,Cucchiari S, Gobio casali L, et al. Bowel frequency in healthy children . Acta Paediatric scand 1989;78:682-4.
12. Khanna V, Podar U, Constipation. Indian Pediatrics; 47: DEC 17, 2012
13. Dehghani SM et al. Middle East J Dig Dis. 2015 Jan;7(1):31-5.
14. Mohanty N, Dutt R. Clinical profile of functional constipation and determining optimam dose of PEG for its successful maintenance therapy (Unpublished data, MGMIHS, 2015)
15. FaleirosFT, MachadoNC Assessment of health-related quality of life in children with functional defecation disorder. Jl de Padiatria; 2006,82(6) 421-425
16. Lakshminarayanan B et al. A new ultrasound scoring system for assessing the severity of constipation in children. Pediatric surgery international 2008, 24(12):1379-84
17. Veras Neto MC et al. Gallbladder motility in children with chronic constipationJPGN; 2008,46(4):414-8 Yanitskaya MY,
18. Sapozhnikov VG gastroenterol, 2015; (1):36- 47
19. Bekkali NL, et al. MRI of LS spine in children with chronic constipation or non retentive fecal incontinence: a prospective study. Journal of pediatrics 2010,156(3): 461-5
20. Schmulson Wasserman M et al. the latin americal consensus on chronic constipation. Gastroenterologia & Hepatologia; 2008, 31(2): 59-74
21. Greg Rubin, Anne Dale. Clinical review of chronic constipation in children BMJ 2006; 333:1051-5
22. Plunkett a et al management of functional constipation in childhood Paed Drugs 2007, 9(1): 33-46
23. Clayden GS et al. Management of chronic constipation and related fecal incontinence in childhood. Arch Dis childhood 2005;90:58- 67
24. Medeiros LC et al. Clinical characteristics of pediatrics patients with chronic constipation according to age group. Arquivos de Gastroenterologia 2007,44(4): 340-4
25. Voskuijl w et al PEG 3350 vs lactulose in treatment of childhood functional constipation: a double blind, randomized controlled multicenter trial Gut 2004;53:1590-4
26. DupontC et al. Double blind rancomized evaluation of clinical, biological toelrence to PEG 4000 Vs lactulose in constipated chindren. JPGN2005; 41:625-33
27. Arik A, Dinesh SP. Polyethylene Glycol: A game change laxative for children. JPGN:57.2:134-140
28. Soares AC et al. Effects of conventional treatment of chronic functional constipation on total, segmental colonic & oro-cecal transit times JI de Pediatr 2009,85(4):355-8
Issue: April-June 2015 [Volume 4.2]
