Role of Serum High Sensitivity C Reactive Protein In Children With Nephrotic Syndrome.
Original Research
Abstract –
Objectives: Nephrotic syndrome (NS) is characterized by proteinuria, edema, hypoalbuminemia and hypercholesterolemia. The latter is a risk factor for atherosclerosis suggesting a higher risk for cardiovascular disease in children suffering from NS. This change is proposed to be due to vascular endothelial dysfunction, reflecting the inflammatory response to tissue damage. One potential inflammation marker high sensitive CReactive Protein (hsCRP) was aimed to be evaluated in these children.
Methods: It is a cross sectional study conducted in tertiary-care hospital predominantly catering to population in Delhi. Forty children with first episode nephrotic syndrome attending the Pediatric Outpatient Department, Vardhaman Mahavir Medical College & Safdarjung Hospital (VMMC&SJH) within 14 years of age and equal no of age and sex matched healthy control children were included in the study. Serum hsCRP was measured by Enzyme linked immunosorbent assay technique. (ELISA)
Result: Serum hsCRP level was elevated in children with NS compared to healthy controls. A positive correlation between serum hsCRP and cholesterol level in cases (r=0.53, p<0.05) was observed.
Conclusion: Children suffering from Nephrotic syndrome are shown with raised hsCRP and positively correlated with hypercholesterolemia. Literature says hypercholesterolemia persists in such patients even after long period remission. It is proposed that regular monitoring serum hsCRP level in such patients may help in understanding role of inflammatory mediated atherosclerosis changes of risk of coronary artery disease in later part of life.
Keywords: hsCRP, Nephrotic syndrome, atherosclerosis, coronary artery disease.
Introduction
Idiopathic nephrotic syndrome(INS) is the common type of nephrotic syndrome in children1.This disease could affect early childhood of both sex2with estimated incidence 9-10 per 100,000 population in Indian subcontinent3. Steroids are cornerstone of treatment. Most patients experience relapse and repeated remission. NS may increase patient susceptibility to infections and causes dyslipidemia in childhood and have a higher risk for cardiovascular disease4. Endothelial dysfunction reflecting the inflammatory response to tissue damage plays a major role in all phases of atherosclerosis 5,6,7 so inflammatory markers are often used as parameters to assess the progress of atherosclerosis. Determination of serum hs-CRP level is currently recommended by the American Heart Association (AHA) in all patients at risk of cardiovascular diseases 8. Serum hs-CRP level below 1 mg/l indicates low risk, 1–3 mg/l average risk, and 3–10 mg/l very high cardiovascular risk 9,10. The aim of the present study was to assess serum hsCRP level to predict the risk of hyperlipidemia related events in patients with NS.
Material And Methods:
This cross-sectional study was conducted in the Biochemistry in collaboration with Pediatrics Department, Vardhaman Mahavir Medical College & Safdarjung Hospital (VMMC and SJH), New Delhi Hospital. Only children (40) with first episode nephrotic syndrome attending nephrology OPD i.e new cases with patients presenting with symptoms for first time and had not taken steroid treatment till now or admitted to wards confirmed as cases of NS and not taken steroid treatment with age ≥1 year and ≤14 years were included in the study. All relapsed cases of NS taking calcium, Vitamin D, diuretics, steroids, having kidney dysfunction, congenital renal anomaly, with persistent hematuria and hypertension, extra renal manifestations suggestive of secondary or systemic causes were excluded from study. Control group consisted of 40 healthy children, age and sex matched not having any signs of acute or chronic disease whose health status was determined through the subjects’ medical history, parental report and routine laboratory tests. In each visit, they were assessed for height, weight, BMI. All samples were collected after 12 h of night fasting. Under strict aseptic conditions venous sample was collected in plain vacutainer. Serum was separated within half an hour of collection and stored at -80 ºC till further analysis. Serum concentrations of hs- CRP, protein, albumin, total cholesterol were measured. The estimation of serum hsCRP was performed by competitive ELISA technique (DLD Diagnostika GMBH, Germany) and serum protein, albumin; total cholesterol estimated in HITACHI 902 autoanalyser. This study was approved by the Ethics Committee. Subject’s parents provided informed consent.
Results:
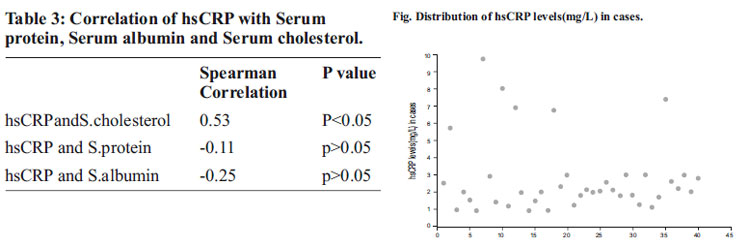
The mean age of children with NS was found to be 8.9 years of which 29 were male and 11female compared to 9.5 years (30 male, 10 female) in control. BMI in cases was 14.9±1.2kg/m2 and 16±2.9 kg/m2in controls. Since there was wide variation in serum hsCRP level median value was calculated. Median serum protein, albumin and cholesterol level was 5.3 g/dl (range,3.5-5.95g/dl), 2.5g/dl(range,1.95-2.9g/dl), 344.35mg/dl (range,165-455mg/dl) in cases and 6.8g/dl (range,6.0-7.9g/dl), 3.8g/dl(3.5-5.1g/dl), 146mg/dl(106-155mg/dl) in controls respectively. Serum hsCRP level in healthy control children showed between 0.25mg/L to 1mg/L with median of 0.56mg/L whereas NS children had markedly elevated level ranging between 0.9mg/L to 9.7mg/L with median of 1.92mg/l.(Table 1).The distribution of hsCRP is shown in Figure 1.Seventy five percent of children had hsCRP level between 1-3 mg/L and fifteen percent greater than 3mg/L. Rest cases had hsCRP level below 1mg/L which is upper margin of control.(Table 2).Further a correlation study between hsCRP and serum cholesterol level showed a significant positive correlation in NS patients. (r=0.53,p<0.05) The cholesterol level was much higher in children with hsCRP level grater then 1mg/L(Table 3).A apparently negative association of hsCRP with serum protein (r= -0.11,p>0.05) and serum albumin (r=-0.25,p>0.05) was found without significance.
Statistics:
The data were analyzed using Graph pad prism statistical software v6. Non-parametric tests were expressed as median, range. Comparison between groups done by Mann Whitney test. Spearman correlation was used to study correlation between variables. P<0.05 was considered significant.
Discussion:
Idiopathic nephrotic syndrome (INS) is the most frequent form of NS in children representing more than 90 percent of cases between 1 and 10 years of age11,12. Male was the predominant gender in both the groups13.
The NS patients were found to have proteinuria and hypoalbuminemia and significantly higher serum cholesterol level than healthy control children.Similar findings were reported by Wasilewska14, Szuminska15et al.in their study. Hypercholesterolemia in NS may be attributed to increase lipoprotein synthesis and decreased catabolism secondary to hypoalbuminemia, increased availability of mevalonate, and decreased activity of Lecithin cholesterol acyl transferase(LCAT), lipoprotein lipase, TG lipase, increased HDL loss in urine 15. Persistenthypercholesterolemia usually leads to atherosclerosis and is associated with endothelial cell dysfunction, elevated oxidant stress, and the creation of a strongly pro-inflammatory condition16.
Several clinical laboratory and pathological findings over the last decades have proved that atherosclerosis is a process beginning in early childhood as the fatty streaks progresses into adulthood 17 resulting to greater risk of coronary heart disease. In susceptible individual, it is obvious that high serum cholesterol level in childhood serves as a nidus for atheroma formation. Kniażewska18et al suggested that nephrotic children have prolonged periods of hyperlipidemia even after clinical remission in children with past history of NS who had completed steroid therapy 4 years to 15 years ago. Similarly, Zilleruelo et al. 19found persistent disorders of lipid metabolism in approximately 50% of patients in the long-term remission period of INS.
Recent evidence has demonstrated that atherosclerosis is not simply a disease of lipid deposition. Inflammation plays a major role in the initiation, progression, and destabilization of atheromas 20,21,22. CRP may be involved in each of these stages by direct influencing processes such as complement activation, apoptosis, vascular cell activation, monocyte recruitment, lipid accumulation and thrombosis23. Large prospective trials have shown hs-CRP to be a strong predictor of future cardiovascular events.24 The connection between hsCRP and atherosclerosis lies on three grounds. First, the concentration of hsCRP in the serum, which is measured by using highly sensitive techniques, correlates with the occurrence of cardiovascular disease. Second, although hsCRP binds only to Fcγ receptor-bearing cells and apoptotic and damaged cells. CRP is able to bind directly to LDL-C particles, especially oxidized (oxLDL) and is deposited in atheromatous plaques. Moreover, its proinflammatory properties further stimulate progression of atheroma. It was shown that even slightly increased hsCRP serum concentration is associated with increased risk of atherothrombotic events in healthy participants 25,26,27,28.
The use of the high-sensitivity test for hs- CRP assessment as an indicator of vascular damage has been recommended by the European Society of Arterial Hypertension since 2003 8. According to the American Society of Cardiac Diseases, increased serum hs-CRP level indicates a risk of cardiovascular incidents 25.Few literature reports concerning the assessment of hs-CRP level in children with nephrotic syndrome who are at risk of developing vascular complications14,29,30. In the present study serum hsCRP level was significantly higher in NS children (median1.92mg/L) compared to healthy controls (median0.56mg/L). Majority of cases presented with hsCRP greater than 1mg/L. Wasilewaska et al had found median hsCRP levels (1.62mg/l, 0.16mg/l) in cases(NS) and control respectively in children 4-14 years. Whereas hsCRP level of 2.03mg/l was reported by other study in NS children 29. Median hsCRP value was 1.5mg/lin patients with NS10 and 2.97mg/l in NS15. Further, we found a positive correlation between serum hsCRP and cholesterol level in cases.Uelandet al. 31assessed hs-CRP in children with familial hypercholesterolemia and observed its significantly elevated serum level.
Conclusion:
It may be inferred from the present study that there is a steep rise in serum hsCRP and cholesterol with a positive correlation among their elevation. In later part of life inflammatory response plays a critical role with a risk of atherosclerosis in such NS children. The most vulnerable groups are those with unremitting proteinuria, frequent relapses and/or poor response to steroids and long-standing hypoalbuminemia 32. Identification of such children may allow early intervention to retard the atherosclerotic process, preventing or delaying cardiovascular diseases. Hence, regular laboratory tests including hsCRP assay and a proper history record of children who had suffered nephrotic syndrome in past is quintessential for a better understanding of pathogenetic factors of the disease, its progression and possible tendency toward atherosclerosis in mere future.
Limitations: It is a cross sectional study including a small population, wider prospective studies including large population including relapse, remission cases and effect of steroids and immunosuppressant’s effect on hsCRP are needed to be studied to strengthen its role. Inclusion of hs- CRP measurement in risk screening and as a preventive measure might result in a marked improvement in prevention of cardiovascular morbidity and mortality in these children.
Contributors: All the authors were involved in designing the study involved in the review of literature, and manuscript preparation and drafting the manuscript. Initial draft of the manuscript was written by Seema Patel. Dr. B.C Kabihas edited, refined and provided critical inputs to the draft manuscript. The final manuscript was approved by all the authors
Funding: None
Competing interest: None stated.
References:
1. Uwaezuoke SN. Steroid-sensitive nephrotic syndrome in children: triggers of relapse and evolving hypotheses on pathogenesis. Ital J Pediatr. 2015;41:19.
2. Davin J-C, Rutjes NW. Nephrotic Syndrome in Children: From Bench to Treatment. International Journal of Nephrology. 2011 Aug 28;2011:e372304.
3. Srivastava R, Bagga A.Pediatric Nephrology. 5/e ed. Jaypee Brothers Medical Publishers(P) Ltd.;2011.
4. Niaudet P, Boyer O. Idiopathic Nephrotic Syndrome in Children: Clinical Aspects. Pediatric Nephrology;2009.667-702.
5. Spagnoli LG, Bonanno E, Sangiorgi G, Mauriello A. Role of inflammation in atherosclerosis.J Nucl Med. 2007 ;48(11): 1800- 15.
6. Tkaczyk M, Czupryniak A, Owczarek D, Lukamowicz J,Nowicki M. Markers of endothelial dysfunction in children with idiopathic nephrotic syndrome. Am J Nephrol.2008;28:197 202.
7. Thakur S, Gupta S, Parchwani H, Shah V, Yadav V. HsCRP – a potential marker for coronary heart disease.Indian J Fundamental and Applied Life Sciences. 2011;1:1-4.
8. Zdrojewski T, Chwojnicki K, Bandosz P, Konarski R, Wyrzykowski B. Distribution of Creactive protein and its relation to arterial hypertension in a country representing a highrisk region for cardiovascular diseases. Blood Press. 2006;15(1):20-6.
9. Pfutzner A, Forst T. High-sensitivity C-reactive protein as cardiovascular risk marker in patients with diabetes mellitus. Diabetes TechnolTher 2006;8:28-36
10. Shostak E, Krause I, Dagan A, Ben-Dor A, Keidar M, Davidovits M. Is serum CRP level a reliable inflammatory marker in pediatric nephrotic syndrome? Pediatr Nephrol. 2016;31(8):1287-93.
11. Kronenberg F. Dyslipidemia and nephrotic syndrome: recent advances. J RenNutr. 2005;15:195-203
12. Nephrotic syndrome in children: prediction of histopathology from clinical and laboratory characteristics at time of diagnosis. A report of the International Study of Kidney Disease in Children,” Kidney International 1978;13(2), 159-65
13. Mubarak M, Lanewala A, Kazi JI, Akhter F, Sher A, Fayyaz A, et al.Histopathological spectrum of childhood nephrotic syndrome in Pakistan. ClinExpNephrol. 2009; 13:589-93.
14. Wasilewska A, Zoch-Zwierz W, Tobolczyk J, Tenderenda E. High-sensitivity C-reactiveprotein (hsHSCRP) level in children with nephrotic syndrome. PediatrNephrol. 2007; 22: 403-8
15. Rybi-Szumi?ska A, Wasilewska A, Michaluk- Skutnik J, Osipiuk-Rem?a B, Fi?onowicz R, Zaj?c M.Are oxidized low-density lipoprotein and C-reactive protein markers of atherosclerosis in nephrotic children? Ir J Med Sci.2015;184(4):775-80.
16. Stapleton PA, Goodwill AG, James ME, Brock RW, Frisbee JC. Hypercholesterolemia and microvascular dysfunction: interventional strategies. J Inflamm (Lond). 2010 Nov 18;7:54.
17. Imakita M, Yutani C, Strong JP et al (2001) Second nation-wide study of atherosclerosis in infants, children and young adults in Japan. Atherosclerosis.2001;155:487-97
18. Kniazewska MH, Obuchowicz AK, Wielkoszy?ski T, Zmudzi?ska-Kitczak J, Urban K, Marek M, et al. Atherosclerosis risk factors in young patients formerly treated for idiopathic nephrotic syndrome. Pediatr Nephrol.2009;24(3):549-54.
19. Zilleruelo G, Hsia SL, Freundlich M, Gorman HM, Strauss J. Persistence of serum lipid abnormalities in children with idiopathic nephrotic syndrome. J Pediatr.1984;104(1):61-4.
20. Mehta JL, Sukhija R, Romeo F, Sepulveda JL. Value of CRP in coronary risk determination. Indian Heart J. 2007 Apr;59(2):173-7.
21. Ross R. Atherosclerosis–an inflammatory disease. N Engl J Med. 1999 Jan 14;340(2):115- 26.
22. Pfützner A, Schöndorf T, Hanefeld M, Forst T. High-Sensitivity C-Reactive Protein Predicts Cardiovascular Risk in Diabetic and Nondiabetic Patients: Effects of Insulin- Sensitizing Treatment with Pioglitazone. J Diabetes Sci Technol. 2010 May 1;4(3):706-16.
23. Shrivastava AK, Singh HV, Raizada A, Singh SK. C-reactive protein, inflammation and coronary heart disease. The Egyptian Heart Journal. 2015 Jun 1;67(2):89-97.
24. Yu H, Rifai N. High-sensitivity C-reactive protein and atherosclerosis: from theory to therapy. Clin Biochem. 2000 Nov;33(8):601-10.
25. Singh SK, Suresh MV, Voleti B, Agrawal A. The connection between C-reactive protein and atherosclerosis. Ann Med.2008 ; 40 (2): 110-20.
26 Pasceri V, Willerson JT, Yeh ETH. Direct proinflammatory effect of C-reactive protein on human endothelial cells. Circulation. 2000;102:2165-8.
27. Labarrere CA, Zaloga GP. C-reactive protein: from innocent bystander to pivotal mediator of atherosclerosis. Am J Med. 2004;117:499-507.
28. Verma S, Devaraj S, Jialal I. Is C-reactive protein an innocent bystander or proathe-rogenic culprit? C-reactive protein promotes atherothrombosis. Circulation. 2006;113: 2135- 50.
29. Astuti KD, Muryawan MH, Mellyana O. Correlation between lipid profile and C-reactive protein in children with nephrotic syndrome. Paediatrica Indonesiana. 2015; 55(1):1-6.
30. Stenvinkel P, Lindholm B. C-reactive protein in end-stage renal disease: are there reasons to measure it? Blood Purif.2005; 23:72- 78
31. Ueland T, Vissers MN, Wiegman A, Rodenburg J, Hutten B, Gullestad L, Ose L, Rifai N, Ridker PM, Kastelein JJ, Aukrust P, Semb AG. Increased inflammatory markers in children with familial hypercholesterolaemia. Eur J Clin Invest.2006; 36:147-152.
32. Marcovina SM, Albers JJ, Dati F et al. International Federation of Clinical Chemistry standardization project for measurements of apolipoproteins A-I and B. Clin Chem. 1991;37:1676-80
Issue: October-December 2017 [Volume 6.4]