Modulation of Cardiac Autonomic tone in Healthy Neonates
Original Research
Corresponding Author: Dr.Ekta Khandelwal, Room No.3119, 3 rd floor,3rd Floor, Department of Physiology, Gate No 5, AIIMS, Tatibandh, Raipur (C.G) 492001, email : khandelwaldrekta@aiimsraipur.edu.in
Received: 23 September, 2019; Reviewed: 30 October, 2019; Accepted: 27, November, 2019.
Citation of article: Sumeet Tripathi , Ekta Khandelwal, Onkar Khandwal, Modulation of Cardiac Autonomic tone in Healthy Neonates in New Indian Journal of Pediatrics, 2019; 8.4. : 178-182
Abstract
Cardiac autonomic tone is beat to beat fluctuation in heart rate. There is paucity of data on normal values of HRV in newborn infants. This study was an initiative to assess the feasibility of measurement and analysis of short term HRV in healthy term neonates. 20 healthy term neonates admitted in Neonatal Unit of Dr BRAM Hospital at Raipur, Chhattisgarh, who met the inclusion criteria of gestational age > 37 weeks & APGAR score >= 8 at 5minutes were included. Cardiac autonomic modulation was assessed by short term heart rate variability by 5 minutes continuous recording of ECG using a lead II electrocardiogram (ECG). The analysis of HRV was done by Time domain, Frequency domain and Non Linear methods. Time Domain values were expressed in first quartile and third quartile of SDSD were between (10.78 – 36.43ms), RMSSD were (10.82 – 36.4) ms and pRR50 and (0.39 -16.82). Frequency domain values expressed in first quartile and third quartile of LF were (56.04 – 72.97 n.u.) , HF were (26.76 – 41.58 n.u). Value of the LF/HF ratio is (1.33- 2.72). Non linear values expressed in first quartile and third quartile of SD1 were between (7.62 – 25.76 ms) & SD2 were ( 25.50-46.03 ms). This study showed recording of heart rate variability in neonates is feasible. It can be a promising noninvasive diagnostic and prognostic tool in the assessment of neonatal and infant diseases.
Key words: Short term HRV, Neonates, Cardiac autonomic tone, ANS
Introduction:
Cardiac autonomic tone commonly known as Heart rate variability (HRV) is beat to beat fluctuation in heart rate (i.e. in R-R intervals) within physiological limit under resting conditions. These beat to beat variations occur due to continuous changes in the cardiac autonomic sympathetic and parasympathetic outflow to the heart.Heart rate variability is now one of the most frequently used non invasive method in scientific study for assessment of sympatho-vagal balance(Cardiac autonomic tone) in health and disease condition.1
Till two decade ago heart’s rhythm fluctuation were ignored in practical cardiology and it was believed that irregularity of cardiac function is a pathological phenomenon. Thus, an observation that an absolutely regular sinus rhythm can also be a negative prognostic factor came as a surprise to many clinicians and cardiologists. The beat-to-beat variation having intrinsic oscillations reflects a complex interplay between ionic membrane current responsible for SA node automaticity and the regulatory influences of autonomic nervous system. In absence of autonomic innervations to heart (as occurs in transplanted heart), there is absolute regularity of heart rate with minimal variations.2-4
In 1960’s after the introduction of electronic fetal monitoring system, the tracing and appreciation of subtle fluctuations existing in the basal HR became possible. Clinically, normal or average baseline variability is considered as a valid indicator of fetal well being5 with increasing knowledge of dealing with measurement and physiological interpretation, HRV is rapidly gaining importance for its clinical application but its role to neonates is still not yet well established. Normal values of HRV in newborn infants are not widely available. This problem may be partially attributed to the lack of standardization of different methods. This study was just an initiative to see the utilityand feasibility to establish short term HRV measurement in clinical practice in healthy term neonates and to record and analyze the normal HRV data of newborn. It’s just a small initiative to further explore the potential of this non invasive tool of cardiac autonomic tone detection into a bigger value like early detection of sepsis, neurodevelopmental outcomes in hypoxic ischemic encephalopathy patients.
Material & Method:
The present study was conducted in the Department of Physiology AIIMS Raipur and Department of Pediatrics, Neonatal Unit& Physiology at Pt. JNM Medical College and associated Dr BRAM Hospital at Raipur, Chhattisgarh, India during, from July 2015 to December 2015 after obtaining ethical clearance from institutional ethics committee. 20 healthy term neonates who met the inclusion criteria ofgestational age > 37 weeks & APGAR score >= 8 at 5minutes were included in the study and patients with major congenital anomalies, obvious cardiac anomalies & Illness requiring admission in neonatal intensive care unit were excluded in the study. After explaining the detail protocol to the parents and taking the parental consent, questionnaires were asked, relevant data were obtained from medical records and following parameters were noted like gender, type of delivery, no of maternal pregnancy (Vaginal delivery, Caesarean section, abortions), gestational age at birth, birth weight, weight at time of evaluation, APGAR at first and fifth minute, age in hours of life at the time of evaluation. Baseline Parameters like pulse rate, respiratory rate, temperature were recorded in all subjects. Cardiac autonomic modulation was assessed by short term heart rate variability by 5 minutescontinous recording of ECG using a lead II electrocardiogram (ECG). Though, in principle, the heart rate variability can be measured over any length of recorded ECG, as per the guidelines of Task Force (1996) at least 5 minutes of ECG must be recorded to quantify Sympathetic and Parasympathetic tone.ECG and Respiration was recorded on 8-channel digital physiograph (Labchart, ADI, Australia).The ECG signal is continuously amplified, digitized and stored in the computer for offline analysis.Processing of acquired ECG signal i,e. detection of R wave (R wave detection and RR intervals) is done by software. Allsoftwaresutilized for recording HRV have basic similarity in that they all compute R-R intervals after the R wave detection, R-R intervals (ms) are plotted against time (sec) to obtain tachogram.
The analysis of HRV was done by three methods: Time domain, Frequency domain and Non Linear methods. Time domain method wasapplied to quantify the variations in RR intervals and the following parameters are computed:
1. SDSD- Standard deviation of differences between adjacent RR intervals.
2. RMSSD- Root square of the mean of the sum of the squares of differences between adjacent RR intervals.
3. pNN50 -Percentage of NN50 (NN50 Number R-R interval differences = 50 ms).
Majority of the conventional time domain parameters (i.e. SDSD, RMSSD, NN50 and pNN50) are markers of parasympathetic activity.
The frequency domain components of HRV were analyzed by using Fast Fourier Transform (FFT). The power spectrum is divided into two frequency bands: LF- (0.040 to 0.15) Hz and HF- (0.15 to 0.4) Hz.
Nonlinear Methods the Poincare plot is a scatter plot of the current R-R interval against the R-R interval immediately preceding it (R-Rn vs RRn+ 1).The analyzed parameters of Nonlinear methods were SD1 &SD2.
Timegiven for newborn to adjust the new environment as resting state was needed.
Newborns were breast fed30 minutes prior to the recording. Comfortableposition for the newborn was ensured.All the recordings were done in a quiet room with an ambient temperature maintained between 27-29°C in the morning between 9 am to 11 am to exclude the effect of circadian rhythm in HRV. The ECG signal was continuously amplified, digitalized and stored in the computer for offline analysis.SPSS software, version 22 was utilized for performing statistical analysis. All the parameter data were reported as means ± SD, medians, and first quartile and third quartile showing frequency distribution of data.
Result:
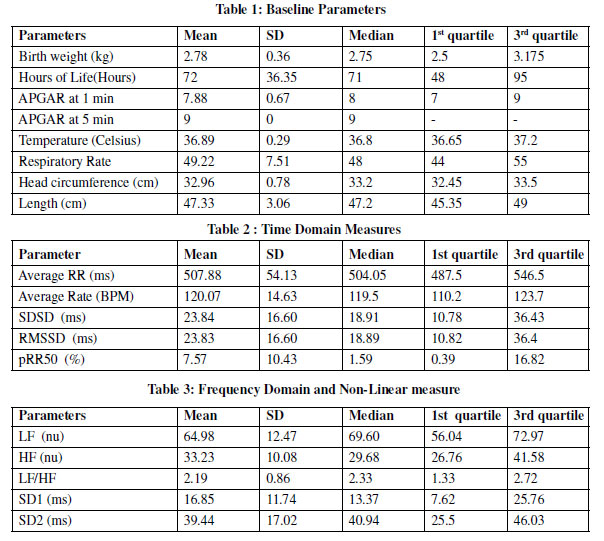
The study was conducted in 20 healthy term infants who were admitted in neonatal unit of Dr BRAM Hospital, Raipur from July 2015 to December 2015. The baseline parameters included birth weight, postnatal age (hours of life), APGAR score at 1 min and 5 min of life, body temperature (Celsius), respiratory rate and the anthropometric measurement of head circumference and length (cm) was calculated.
The mean birth weight of neonates in the study was found to be 2.78+/- 0.36 kg while the mean age was 3 postnatal days (72 hours). No gross deviation were observed in head circumference and length measurements from the normal range described for neonates. The temperature and respiratory rate of the neonates in the study lied within the normal range described for neonates. (Table 1)
The average RR interval was between 487.5 – 546.5 ms, the average heart rate was between 110.2- 123.7 bpm lying well within physiological limits of the newborns. The HRV parameters included in this study were time domain, frequency domain and nonlinear analysis. Time Domain values were expressed in first quartile and third quartile of SDSD were between (10.78 – 36.43ms), RMSSDwere (10.82 – 36.4) ms and pRR50 and (0.39 -16.82). (Table2)
Frequency domain values expressed in first quartile and third quartile of LF were (56.04 – 72.97 n.u.) , HF were (26.76 – 41.58 n.u). Value of the LF/ HF ratio is (1.33- 2.72).
Non linear values expressed in first quartile and third quartile of SD1 were between (7.62 – 25.76 ms) & SD2 were ( 25.50-46.03 ms). (Table 3)
Discussion:
Heart rate variability is one of the most frequently utilized tool to assess cardiac autonomic modulations by analyzing the spontaneous variability of continuous series of R-R interval (in an ECG) recorded under resting conditions.HRV reflects the response of ANS to intrinsic and extrinsic stimuli. Continuous changes in sympathetic and parasympathetic neural impulses leads to alterations in the heart rate and causes oscillations around the mean value, what is referred to as HRV. Heart rate variability studies provides an opportunity to understand the dynamic nature of heart functions and ANS functionality.6-7
Earlier literature mentioned that the ratio of the power in the low frequency band to that in the high frequency band seems to decrease with gestational age and thus correlates with autonomic nervous system maturation in infancy.8HRV can be of special importance especially in preterms as it can help in understanding the developmental changes cardiac autonomic tone. Thus, it can be used as important tool for assessing maturation of autonomic nervous system in preterms at birth and with increasing postnatal age.
Extracting the clinical significant features of HRV under various conditions, might help us understand the pathophysiology of derangement of autonomic function. It can help in better understanding of imbalance in homeostasis and disease mechanism.9 Studies have shown the clinical importance of HRV in neonates. Some studies propose grading of HIE using HRV in neonates. Also it may be used as a tool for early warning system for brain injury in neonates in remote areas where the EEG is not readily available.10-11 In neonates decreased HRV has been associated with sepsis. A state of decreased overall variation, lower LF variation, and decreased complexity has been shown to consistently correlate with the presence and severity of systemic infection.12-14
But further research is needed to compare the prognostic and diagnostic value and clinical utility of the various traditional and new HR variability measures in neonates before an ideal index can be introduced for clinical intervention purposes. Heart rate variability, by far remains a very promising noninvasive tool for assessment of cardio-vagal tone in health and disease conditions of newborns.
In conclusion this study showed recording of heart rate variability in neonates is feasible. However, at present, lack of standard criteria for the analysis of heart rate variability, prevents precise comparisons among the various studies. Until recommendations for standardized analytical methods are made, clinical application of heart rate variability in neonatal and infant prognosis and therapy would remain premature.
Contribution of authors:
1. Dr Sumeet Tripathi- Literature search & design of study, manuscript preparation
2. Dr Ekta Khandelwal- Recording and Analysis of data, proof reading
3. Dr Onkar Khandwal- Statistical analysis and patient management, manuscript preparation
Conflict of Interest: None
Funding: None
Acknowledgement: All the mothers of subjects included for their cooperation.
References:
1. Heart rate variability: standards of measurement, physiological interpretation, and clinical use. Task Force of the European Society of Cardiology and the North American Society of Pacing and Electrophysiology. Circulation. 1996;93(5):1043-65.
2. Malik M, Camm John A,Heart rate variability,Armonk,NY. Futura Publishing Company,Inc 1995
3. Harald M. Stauss Heart rate variability. Am J PhysiolRegulIntegr Comp Physiol 2003; 285: 927–31.
4. Luiz Carlos Marques Vanderlei, Carlos Marcelo Pastre, Rosângela Akemi Hoshi, Tatiana Dias De Carvalho, MoacirFernandes De Godoy. Basic notions of heart rate variability and its clinical applicability. Rev Bras Cir Cardiovasc.2009; 24(2): 205-17.
5. De Haan J, Van Bemmel JH, Versteeg B, et al. Quantitative evaluation of fetal heart rate patterns. Eur J ObstetGynecol 1971;1:95
6. Denton TA, Diamond GA, Helfant RH, et al. Fascinating rhythm: a primer on chaos theory and its application to cardiology.Am Heart J 1990;120:1419-1440
7. Molgaard H, Sorensen KE, Bjerregaard P. Circadian variation and influence of risk factors on heart rate variability in healthy subjects. Am J Cardiol 1991;68:777-784
8. Udi Chatow, Davidson S, Reichman B L, And Akselrod S Development and Maturation of the Autonomic Nervous System in Premature and Full-Term Infants Using Spectral Analysis of Heart Rate Fluctuations Vol. 37, No. 3, 1991
9. Malarvili M B, Mesbah M, and Boashash B. Time-Frequency Analysis of Heart Rate Variability for Neonatal Seizure Detection EURASIP Journal on Advances in Signal Processing Volume 2007, Article ID 50396,
10. Aliefendioglu D, Dogru T, Albayrak M, Dibekmisirlioglu E, Sanli C (2012) Heart rate variability in neonates with hypoxic ischemic encephalopathy. Indian J Pediatr 79(11):1468– 72
11. Vladimir Matic, Perumpillichira J. Cherian, DevyWidjaja, Katrien Jansen ,Gunnar Naulaers, Sabine Van Huffel, and Maarten De Vos, Heart Rate Variability in Newborns with Hypoxic Brain Injury
12. Godoy, J López, L Bermúdez, A Ferrer, N García, C GarcíaVicent, EF Lurbe, J SaizTime- Domain, Frequency Domain and Non-Linear Measurements in Neonates Heart Rate Variability with Clinical Sepsis
13. Griffin MP, et al. Heart rate characteristics and clinical signs in neonatal sepsis. Pediatr Res 2007; 61: 222-7.
14. Moorman JR, et al. Cardiovascular oscillations at the bedside: early diagnosis of neonatal sepsis using heart rate characteristics monitoring. Physiological Measurement 2011; 32: 1821.
Issue: October-December 2019 [Volume 8.4]