Benign Acute Childhood Myositis Occuring in Clusters in Navi Mumbai; Presenting with Fever, URTI, Muscle Pain, Raised Muscle and Liver Enzymes
Case Report
Abstract:
Three migrant children residing in the same locality presented to our paediatric OPD on the same day in June, 2016 with fever, cough and cold, followed by severe pain in the lower limbs; unable to take weight and stand. The pain was acute in onset in all children, falling in the age group of 5 to 7 years. There was no apparent neurological deficit – sensory nor motor. Tone and power in both limbs were essentially normal. All of them had normal haemoglobin, WBC and platelet counts. However, their muscle and liver enzymes were typically raised in all, normalizing within a week. Nerve conduction studies were normal. We report a series of cases clinically suggestive of acute benign childhood myositis (Viral), occurring in a cluster in the sub-urbs of Navi Mumbai, among migrant children who apparently had poor immunity against the disease, possibly been recently introduced in the region.
Key words:
Benign acute childhood myositis, hypertransaminasemia, Raised CPK, Viral myositis
CASE -1
A five year-old male child ‘A’ residing at semiurban of Navi Mumbai; hailing from Pune. Was brought with complaints of fever since 4 days, cough and cold since 2 days, severe pain in both legs since 1 day and difficulty in walking since few hours. The child was apparently alright 4 days back when he developed remittent fever which was of mild to moderate grade, not associated with chills/rigor. Fever used to relieve on oral paracetamol. He also had mild cough that was dry, intermittent, having no diurnal or postural variation. A local practitioner prescribed him oral azithromycin for 2 days. However, he complained moderate to severe pain in legs on day-3 night but was able to bear weight to stand. Had difficulty in standing since morning (Day-4) and even complained of pain on touching the leg muscles.
His general physical condition was fair. He was febrile with pulse rate 108 per minute, regular, peripheral pulses well felt, BP-110/80 mmHg, respiration rate 26/min. No pallor, jaundice or lymphadenopathy. Anthropometry was appropriate for age.
P/A: Soft, non-tender, liver 3 cm enlarged below right costal margin (Span 12 cm), spleen not palpable, no free fluids. CVS, R/S normal. Conscious, oriented to time, place and person. No meningeal signs No neurological deficits. Both calf muscles were tender, even on light touch. There was no swelling, redness or change in local temperature.
Child was admitted and given symptomatic treatment, maintenance fluid and rest. Routine investigations, including CBC, liver enzymes and CPK were sent. He improved gradually over next 3 to 4 days.
CASE -2
Seven year old male child Y, residing at semiurban area of Navi Mumbai, hailing from Andhra Pradesh was brought with c/o Fever since 7 days, Cough and Cold since 2 days, pain in both legs since 1 day and difficulty in walking since midnight. He was apparently alright 7 days back when he developed fever which was documented as mild to moderate grade, associated with chills but no rigor; 1-2 spikes in a day, relieved on medication. The child had mild cough that was dry, intermittent, with no diurnal or postural variation. Child had body-ache and headache at the height of fever. He received oral antibiotic (Amoxyclav) for 2 days initially. Patient complained of pain in both legs on day-5, but was able bear weight. Unable to stand since mid-night; had intense muscle pain throughout night.
On examination, the child was febrile with temperature 380 C, pulse 92/min, all peripheral pulses well felt, BP-100/78 mmHg, RR 24/min. No pallor, jaundice, lymphadenopathy. Anthropometry was appropriate for age.
P/A: Soft, non-tender. Liver enlarged, 3cms BCM(R), span 13 cms. Spleen palpable 1cm BCM (L)
CVS – NAD, R/S – Clinically clear. Child fully conscious, well oriented. No meningeal sign. No neurological deficit. On local examination of legs, calf muscles and thighs of both lower limbs were tender on touch. However, there was no swelling or redness or raised local temperature.
The child was admitted and given maintenance intravenous fluids, symptomatic treatment for pain (Paracetamol) and rest. Routine investigations, liver and muscle enzymes (CPK, levels were sent .Patient was improved gradually over next 3-4 days.
CASE -3
Seven year old male child AR, a known case of autism with mild intellectual disability, residing at semiurban of Navi Mumbai; hailing from Tamilnadu, was brought with complaints of fever for last 4 days and limping for 1 day. There was no history of motor weakness ever earlier. Patient was apparently alright 4 days back when he developed fever which was acute in onset, of mild to moderate grade, not associated with chills/ rigor. Fever was remittent in nature with 1 to 2 spikes in a day, relieved on medication (Paracetamol). The child started limping while on day 4 of fever, which gradually worsened. He started dragging his feet more in the right side while walking. No history of coryza, cough. No urinary symptoms, photophobia, nausea, vomiting, diarrhea, seizures, altered sensorium.
On examination, his general condition was fair. He was febrile (Axillary temperature 38.5o C. Pulse rate 90/min, all peripheral pulses well felt, BP 100/70 mm Hg and respiration rate 22/min.
There was no significant pallor, jaundice or lymphadenopathy. Abdomen was soft, non-tender; liver was not enlarged and spleen was not palpable. CVS – NAD; Respiratory system- clinically clear. Child was fully conscious, and well oriented. Calf muscles of both legs were tender to even touch. There was no swelling / redness / local rise in temperature.
Child was admitted and was given maintenance intravenous fluids as food intake was poor. He was given symptomatic treatment (Paracetamol) for pain. Appropriate investigations such as – CBC, M.P., LFT, RFT, muscle enzymes were sent. Nerve conduction studies in lower limbs found to be normal. The patient improved gradually and was able to walk in next 4 days; discharged with follow-up advice and physiotherapy.
Table-1. Summary of Clinical Presentations:

All 3 cases reported from same contiguous area of their current residence, presenting with viral like illness at the same day (Timing). Significantly, all the 3 were migrants from far off places, possibly having no antibody against the suspected virus causing the illness.
Table-2. Summary of Investigations Carried Out:
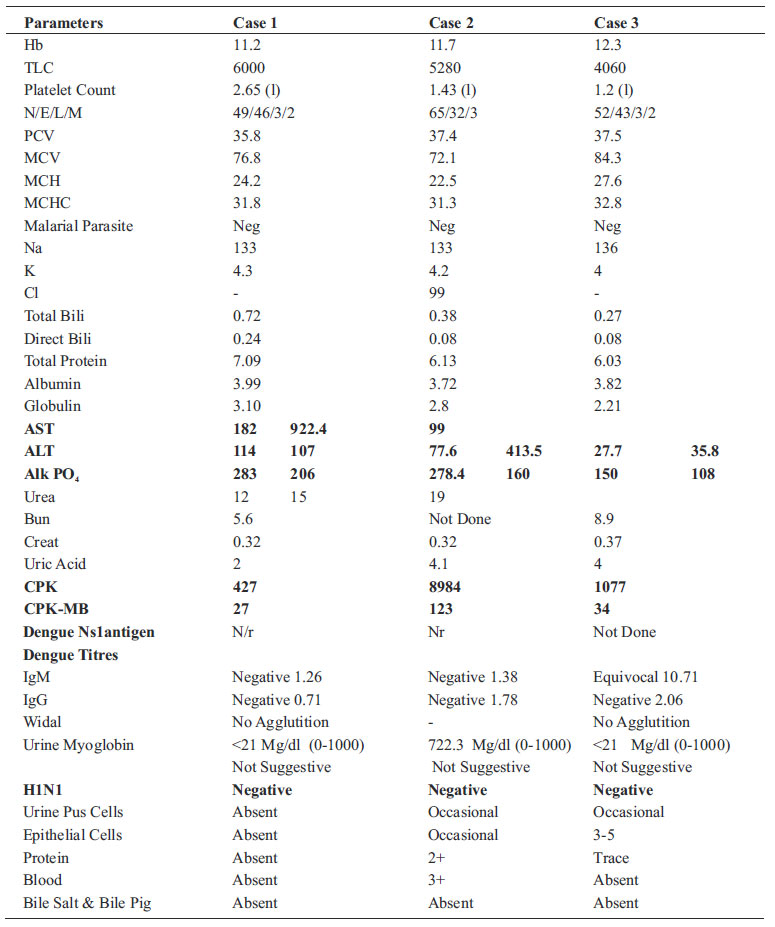
Muscle and liver enzymes were significantly raised in all except near normal ALT in case no. 3. However, due to non-availability of specific probes, virus characterization could not be done.
Course in Hospital :
All the patients were treated as viral myositis with bed rest, iv fluids and symptomatic management with antipyretics (Paracetamol) to which they responded very well.
All of them improved within a day or two. They started bearing weight within 36-48 hours started walking with significnt reduction in pain to no pain soon thereafter.
Discussion :
Acute muscle pain and difficulties in walking could be suggestive of both benign and severe degenerative diseases. Daily physical examination and urine dipstick are sufficient to confirm diagnosis of benign acute childhood myositis (BACM) and to rule out severe complications and other degenerative diseases. 1
Benign acute childhood myositis (BACM) manifests with viral URI like illness, sudden onset of muscle pain, often in the calves and consequent walking difficulty.2,3,4,5 It is often not correctly diagnosed but thought of a rare and severe muscle disease.3,6,7 Proper medical history and clinical examination help in correct diagnosis, avoiding unnecessary and complex tests. The condition is seldom reported in medical literature.
Vito T. et al in 2014 reported1 a similar case of a 7 year old boy having sharp calf pain and progressive walking difficulty, preceded by fever, cough, malaise and rhinorrhea 2 days back. There was no history of neuromuscular disorders in past. The child had taken all mandatory vaccines. No history of travel, trauma, vigorous exercise or similar episodes reported earlier. Muscle power, tone and deep tendon reflexes were normal in all limbs. At rest, the patient kept his feet in slight plantar flexion. Calf muscles on both sides were soft on palpation, no redness or any local rise of temperature. Passive dorsiflexion of the ankles caused sharp pain as well as passive stretching and gentle palpation of his calves. The patient was hospitalized for observation and to exclude any severe connective tissue or muscle disorder. His creatinine phosphokinase was (2161 U/L, normal range <227 U/L), alanine transaminase (69 U/L, normal range: 0-45) and aspartate transaminase (92 U/L, normal range: 17-59). C-reactive protein (<0.20 mg/L) and white blood cell count (7400/?L). CBC, electrolytes, BUN, creatinine, prothrombin time, partial thromboplastin time were all within normal limits. Urine examination revealed no myoglobulin, blood or proteins. Throat culture was positive only for commensal bacteria. Tests for influenza A/B and H1N1 influenza A was negative. Furthermore, serological tests ruled out recent viral infections by adenovirus, respiratory syncytial virus, cytomegalovirus, herpes virus and Epstein- Barr virus, as well as serological tests for mycoplasma pneumonia. Since the patient refused to eat and drink, he was given intravenous fluids for a day. By next day, his pain spontaneously resolved and had normal gait. Child did not present any neurological sequelae on follow-up.
Common viral infectious infections which may present with myositis are as under:
1. INFLUENZA MYOSITIS (A / B; H1N1)
- Childhood form
- Fever, malaise, and rhinorrhea followed 1-7 days later by severe pain, especially in the calves
- Muscle pain worse with movement, especially with walking
- Symptoms of myositis – Generally last 1-7 days
- Involvement of the gastrocnemius-soleus muscles causes calf pain and difficulties with walking( Toe-walking, broad-based gait)
- Complications include myocarditis and respiratory dysfunction.
- Adult form
- Fever, myalgias, generalized weakness
- Muscle swelling in some patients
Laboratory investigations :
- Elevated CK, mostly consisting of the MM (Muscle) isoenzyme, as high as 500 times of normal
- Urine myoglobin may be positive
- Liver enzymes (Aspartate aminotransferase [AST] and lactate dehydrogenase [LDH]) – may be elevated
- Electrocardiogram remains essentially normal
- Detection of virus with polymerase chain reaction (PCR) testing of nasopharyngeal specimens helpful in pin-pointing the exact virus.
2. DENGUE MYOSITIS
Dengue is the most common and widespread arthropod-born arboviral infection. Symptoms include fever, headache, muscle and joint pains and a characteristic skin rash.
Though myalgias are common but myositis and/or elevated serum creatinine kinase is an uncommon complication of dengue virus infection.
3. STREPTOCOCCAL MYOSITIS
- Most common form is group A streptococci (GAS) necrotizing myositis / streptococcal myonecrosis
- Usually seen in the men and young adults
- Spontaneous occurrence (no history of penetrating trauma) or in the immunocompromised
- Evolves to severe local muscle pain, swelling, and fever
- Rapidly progressive and can be fatal
- Complications – Bacteremia, toxic shock syndrome, multiorgan failure.
Laboratory investigations:
- Leukocytosis
- Elevated muscle enzyme levels
4. PYOMYOSITIS
- Psoas abscess – Subtle symptoms such as fever and flank, hip pain; may manifest as pyrexia of unknown origin; may be primary (No identifiable source of infection / spread from occult hematogenous) or secondary (Spread from infection in vicinity)
- Occur mostly in the immunocompromised
- Present with fever and malaise
- Muscles are painful, swollen, tender, and indurated.
- Quadriceps muscle is involved most commonly.
- The second most common location is the psoas muscle, followed by the upper extremities.
Laboratory investigations :
- Leukocytosis, Elevated erythrocyte sedimentation rate (ESR)
- Serum creatine kinase (CK) and aldolase usually normal
- Blood culture results generally negative
- Purulent material for Gram stain, anaerobic and aerobic cultures, antimicrobial sensitivity testing
5. TRICHINOSIS
- Cardinal features – Myalgia, periorbital swelling, and fever (Image)
- Depending on site of involvement – Diplopia, dysarthria, dysphagia, dyspnea
- Eosinophilia is suggestive of the diagnosis.
Laboratory investigations :
- Leukocytosis, elevated immunoglobulin E, and increased muscle enzymes.
- A rising antibody titer is highly suggestive of the disease
6. LYME MYOSITIS
- Symptoms in the vicinity of skin lesions or in limb muscles
- Weakness and atrophy of the proximal muscle groups can occur, accompanied by local swelling and tenderness.
- Muscle weakness may be a major presenting feature of this disease.
- Rarely, late ocular involvement, including orbital myositis , may occur.
7. CYSTICERCOSIS WITH MYOSITIS
- Fever, myalgias
- The most common sites of involvement are the skeletal and cardiac muscle, brain, and eyes
- When skeletal muscles are involved, palpable cysticerci (mature larvae) appear in subcutaneous tissues.
- A notable feature of this type of myositis is muscle pseudohypertrophy, which may be seen in the tongue or calf muscles.
- During the acute stage of disease, patients may have fever and muscle tenderness.
8. TRYPANOSOMIASIS WITH MYOSITIS
- Acute stage
- May be asymptomatic or characterized by fever
- Myositis occurring in the early stage of infection – Symptoms such as muscle weakness and myalgias mimicking those of polymyositis.
- Characterized by fever, lymphadenopathy, and hepatosplenomegaly.
- Chronic stage – Myalgias
- At the site of the insect bite, local inflammation results in a swelling known as a chagoma.
- Contamination of the eyes produces unilateral periocular and palpebral edema with conjunctivitis and preauricular lymphadenopathy (Romaña).
- Extraocular involvement is rare. It may present with features of subacute orbital myositis and may mimic an orbital tumor.
- During the acute parasitemic stage, intense infection of the myocardium may occur, producing severe myocarditis and disturbances of cardiac conduction.
- Clinical manifestations in the early stage of myositis include muscle weakness, tenderness, and erythema mimicking those of polymyositis and dermatomyositis.
- Skeletal muscle may be involved in the chronic stage as well and can last for decades.
9. TOXOPLASMA MYOSITIS
- Fever, myalgias, and muscle weakness
- Polymyositis is a prominent feature even in the congenital form of toxoplasmosis
10. ACUTE COXSACKIEVIRUS MYOSITIS
- Group A virus infection – Myalgias, weakness
- Group B virus infection – Causes epidemic pleurodynia (Bornholm disease or epidemic myalgia), which is considered a form of myositis
- This is an acute, febrile disorder with abrupt onset of pain in the abdomen or lower thoracic region.
- Pain can be referred to the back and shoulders.
- Pain is worse with movement, breathing, or coughing.
Laboratory investigations:
- Rising coxsackievirus IgG antibody titers
- Isolation methods for group B coxsackievirus – Include inoculation of cell cultures
11. FUNGAL MYOSITIS
- Most often seen in severely immunosuppressed patients
- Clinical presentation is similar to pyomyositis
12. CRYPTOCOCCAL MYOSITIS
- Rare cause of myositis
- Most involve immunocompromised patients.
- Symptoms overlap those of bacterial myositis.
- Often present with lower extremity pain and swelling
- May involve the paraspinal musculature
Differential Diagnosis:
Acute Inflammatory Demyelinating Polyradiculoneuropathy, Chronic Inflammatory Demyelinating Polyradiculoneuropathy, Femoral Mononeuropathy, Metabolic Myopathies, Neuromuscular and Myopathic Complications of HIV, Paraneoplastic Autonomic Neuropathy

In associated HIV, symmetric lower limb ascending weakness in a few may be seen.
Treatment of Viral myositis:
- Treatment comprises bed rest, intravenous fluids, and symptomatic management with antipyretics and analgesics.
- Antiviral agents such as amantadine could be considered in adults
Benign acute childhood myositis
It is a self-limiting condition, frequently affects gastrocnemius and soleus muscles. In a review of 316 cases of influenza-associated myositis 5, other causal agents such as- enterovirus, mycoplasma pneumonia and dengue virus have been implicated.3,8 Five cases of BACM following H1N1 influenza A virus infection6,7 and human para-influenza virus type 1 infection9 reported. It is reported that 10 of 316 children (3%) however developed severe rhabdomyolysis, and dialysis was necessary in six cases.5 During winter of 2007- 2008, influenza B virus was responsible for a large number of cases of BACM in Germany, especially among male children aged from 6 to 9 years.3 Median time between onset of fever and the beginning of BACM symptoms was 3 days. Despite the clinical course of BACM being well described, Mall et al. showed that only 24% of 165 participating physicians were able to recognize BACM. 3 The incidence, prevalence and pathogenesis are not known to many even now. BACM has also been described in adolescents.8 This could simply be explained by the increased tropism of viruses for immature muscle cells.3 Each virus could act as a trigger in genetically predisposed children and in few patients with undiagnosed metabolic conditions.3, 7
No invasive tests or medicine therapy really needed. Onset may however be mistaken for serious neurological illness e.g.- Guillain Barrè syndrome or chronic autoimmune diseases. Hence unnecessary tests, such as – radiography, echocardiography, electromyography and magnetic resonance are still performed.3,8,9 Daily clinical status and urine dipstick for myoglobin are sufficient to monitor complications and rule out severe illnesses. Creatinine kinase (CK) should be measured only at initial diagnosis in order to exclude degenerative conditions as the levels do not correlate with severity.3 Tests for related viruses need not be routinely done in view of time lag between infection and sero-conversion. Neither etiological agents are always detected nor antiviral drugs routinely recommended. At the most, influenza test may be useful as these viruses may affect severity of BACM.10, 11
A regional outbreak of influenza virus Bassociated ‘Myalgia cruris’ was observed during seasonal influenza outbreak observed in Switzerland12 in 2013. In a prospective study among the Swiss-Italian pediatric units and pediatricians, diagnosis of myalgia cruris was made in 49 children aged 3.0-14 years (?:?=1.7). Flu-like symptoms were resolving when bilateral calf pain began but remitted in 7days. The creatine kinase-level, was elevated in 25 out of 28. Nose swabs were positive for influenza virus B in 13 of 14 cases. CBC in 41 cases, leucopenia found in 12 and thrombocytopenia in 3. The review of the literature found 10 outbreaks of 10 cases of influenza virus B-associated myalgia cruris, which included a total of 203 patients with a mean age of 7.3 years and a ratio of 2.0. In conclusion influenza virus B caused a large Swiss-Italian outbreak of BACM. Influenza virus B-associated BACM affects preschool- and school-aged children, primarily boys.
Once symptoms resolved, patient does not require any follow-up. However, parents should be encouraged to monitor the child’s urine output and the appearance of Cola colored urine and swollen legs. Hospitalization should be scheduled only when the patient’s parents do not seem able to monitor the condition of their child at home, as was done in our cases. The typical symptoms and signs which can help clinicians to make a correct differential diagnosis when a child suffers from acute muscle pain. BACM typically manifests with acute myositis and increased CK level, following a viral infection. A family history of neuromuscular disorders, myoglobinuria, trauma, chronic progression, rash, edema, muscle weakness or neurological diseases are not typically associated to BACM; in these cases further investigation is required.
References:
1. Vito Terlizzi, Federica Improta, and Valeria Raia. Simple diagnosis of benign acute childhood myositis: J Pediatr Neurosc. 2014 Sep-Dec; 9(3):280-282.
2. Lundberg A. Myalgia cruris epidemica. Acta Paediatr. 1957;46:18-31.
3. Mall S, Buchholz U, Tibussek D, Jurke A, An der Heiden M, Diedrich S, et al. A large outbreak of influenza B-associated benign acute childhood myositis in Germany, 2007/2008. Pediatr Infect Dis J. 2011;30:E142-6.
4. Middleton PJ, Alexander RM, Szymanski MT. Severe myositis during recovery from influenza. Lancet. 1970;2:533-5.
5. Agyeman P, Duppenthaler A, Heininger U, Aebi C. Influenza-associated myositis in children. Infection. 2004;32:199-203.
6. Koliou M, Hadjiloizou S, Ourani S, Demosthenous A, Hadjidemetriou A. A case of benign acute childhood myositis associated with influenza A (H1N1) virus infection. Clin Microbiol Infect. 2010;16:193-5.
7. Rubín E, De la Rubia L, Pascual A, Domínguez J, Flores C. Benign acute myositis associated with H1N1 influenza A virus infection. Eur J Pediatr. 2010;169:1159-61
8. Dandolo A, Banerjee A. Benign acute myositis in a 17-year-old boy. Arch Pediatr. 2013;20:779-82
9. Tippett E, Clark R. Benign acute childhood myositis following human parainfluenza virus type1infection.Emerg Med Australas. 2013;25:248-51
10. Swaringen JC, Seiler JG, 3rd, Bruce RW., Jr Influenza A induced rhabdomyolysis resulting in extensive compartment syndrome. Clin Orthop Relat Res. 2000:243-9.
11. Hu JJ, Kao CL, Lee PI, Chen CM, Lee CY, Lu CY, et al. Clinical features of influenza A and B in children and association with myositis. J Microbiol Immunol Infect. 2004;37:95-8.
12. Ferrarini A1, Lava SA1, Simonetti GD1, Ramelli GP1, Bianchetti MG2; Swiss Italian Society of Pediatrics. Influenzavirus Bassociated acute benign myalgia cruris: an outbreak report and review of the literature. Neuromuscul Disord. 2014 Apr;24(4):342-6. doi: 10.1016/j.nmd.2013. 12.009. Epub 2014 Jan 4.
Issue: April-June 2016 [Volume 5.2]
